Fungal toenail infection often imposes a huge cosmetic concern. It can have great detrimental effects on self-esteem and quality of life. So, what do you need to know to avoid/treat this dermatological condition? Learn more about fungal toenail as we go through the risk factors, stages of the infection, and effective fungal nail treatment for both fungal toenail and tinea!

The Risk Factors – what puts you at risk of getting fungal toenail infection
Poor Foot Hygiene
It may seem like a sensitive topic to discuss, but it is important. Poor foot hygiene is the number one risk factor when it comes to fungal toenail infection. Fungi strive in moist environments – sweat-soaked shoes, unchanged socks, in between toes are some of their favourite hang-out places.
Socks need to be changed daily, if not more. If you are prone to having sweaty feet, we would encourage you to try changing your socks during the day. You can do that discreetly by changing your socks in a bathroom at work. Not only will that lower your risk of getting a fungal infection, your feet will actually feel better in a fresh pair of socks! Alternatively, you can spray Tinaderm (an antifungal powder spray) under your feet to keep them drier in shoes.

It is also a good idea to have at least two pairs of shoes that you can alternate from day to day. This allows the shoes to dry out completely before the next wear, reducing your chance of developing a fungal toenail infection.

Foot hygiene also extends to washing your feet thoroughly daily. Our feet can be a bit difficult to get to sometimes, but it is essential to wash them with soap in the shower. Be sure to dry your feet, especially in between the toes, thoroughly afterwards.
Being Barefoot in Public Places
Certain places are pretty much playgrounds for fungi – change rooms, communal showers, and even hotel carpets. Not only is the humidity usually high in those environments, there is a high amount of (bare)foot traffic. Because fungal infection is contagious, it only takes one person to contaminate the environment as they leave their footprints behind. Going barefoot then exposes your feet to picking up the infection.

We are always very cautious when it comes to going barefoot. (“Well, probably because you are a podiatrist.” One would argue) When we travel overseas, or have to use a bathroom that is not our own, we almost never shower without wearing a pair of flip flops. Strange, and maybe a bit over the top, but there is really no need to ourselves at risk!
Cross Infection & Re-Infection
That is when sharing is NOT caring. If your partner, housemates, or family members, has/have untreated fungal infection, it could be problematic. Firstly, you are likely to get the infection because it is contagious. Secondly, you won’t be able to get rid of your fungal toenail infection because you keep getting the infection again and again from your partner/housemates/family members.
Untreated Tinea Pedis – Fungal Infection of the Skin
Many toenail infections start with untreated tinea pedis, a fungal infection of the skin. Fungi in the skin can migrate to toenails and start making themselves home. For your reference, tinea pedis is also known as athlete’s foot.
The presence of red dots, flaky spots and scaliness are common symptoms of a more severe tinea infection.

Going to Nail Salons
Some nail salons, unfortunately, don’t practise good infection control. The instruments they use may be merely washed and scrubbed before they get to your toes.
For instruments to be 100% bacteria and fungi free, proper sterilisation needs to be in place. Take our clinic for example, we use a new pack of instruments for each client. After each use, we wash the instruments first in an ultrasonic cleaner with a medical grade detergent. Then, we dry the instruments and pack them in a sterilisation pouch, a special pouch with seal that allows the instruments to be sterilised and stored properly afterwards.

Ultrasonic cleaner 
Sterilisation in progress in the autoclave 
Freshly sterilised instruments!
After the instruments are packed into individual pouches, we put them in an autoclave. An autoclave uses steam AND pressure to thoroughly sterilise all the instruments. Steam or heat by itself cannot achieve complete sterilisation. And, that’s where most nail salons fall short. Just because the instruments appear hot, it does not mean they are actually sterilised.
Fungal Toenail Infection Can Get Worse Over Time – The Stages
This may sound surprising, but the primary site of fungal toenail infection is actually the nail bed. That is why generally the infection would not simply “grow out” with the toenail. In fact, the opposite happens. The new nail will catch the infection when it grows over the infected part of the nail bed. It will then seem like the nail will always become discoloured no matter how many times you have trimmed it away.
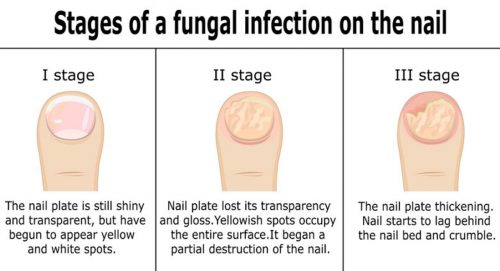
At the early stage of fungal toenail infection, the affected toenail may have a spot of a line of yellow discolouration. Other than that, the nail still looks smooth, shiny, and close to normal.
As the infection progresses, the area of discolouration could extend bigger. You would also notice some change in the texture of the nail. Sometimes you may see mild inflammation in the skin adjacent to the nail. When you try to clean the toenail, there may be some crumbly debris underneath the nail as well.
The next stage of fungal toenail infection will see the toenail lose all its healthy texture. The nail will become thick and very crumbly, much like the texture of a piece of termite infested wood. There is marked yellow, sometimes brown even, discolouration. You would also notice detachment of the nail from the nail bed. Very severe fungal infection would have a very distinct, unpleasant smell.

The general rule is that treatment becomes much more difficult each time the infection progresses. So, remember, early treatment is the key!
What To Do Then – Effective Fungal Nail Treatment
Treating fungal nail infection is not rocket science, but it is nothing short of challenging. While antifungal treatments WORK, what may make someone feel otherwise is the high risk of re-infection and lack of patience to follow through on the treatment.

Identify & Mitigate Risk Factors
The first thing we need to do is to identify and mitigate risk factors. Without doing so, it will always seem like you are moving three steps forward and two steps back. Not only will it lengthen the treatment time, it will inevitably add to your frustration. So, if your partner has tinea, or fungal toenail, get the partner to do the treatment too; avoid going around barefoot; stop getting your nails done at a nail salon; change and wash your socks daily. Whatever the risk factors are for you, mitigate them!
Regular Podiatry Treatment
Like we mentioned before, the infection is actually IN the nail bed. What it means is that if you don’t expose the nail bed, and put antifungal directly on top, the antifungal medication will have a very hard time penetrating the nail (especially when it’s thick), let alone getting to the actual site of infection.

We always trim away any infected parts that are ready to come off, or file down the nail extensively, to expose the nail bed as much as possible. You will need to have regular podiatry treatments (every 4 weeks preferably) to have any infected bits and pieces removed.
Daily Home Treatment
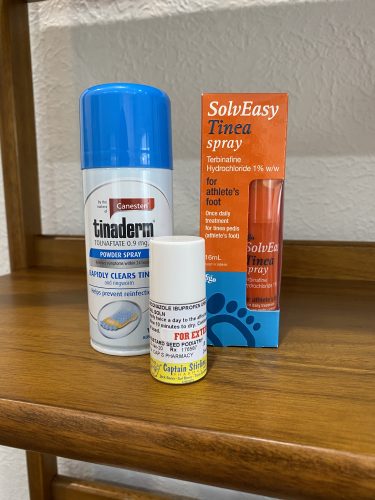
Then, you will need to make it a habit to do the fungal nail treatment at home daily. This includes spraying your feet to clear any tinea, applying an antifungal nail treatment to the affected nails, and spraying your shoes with an antifungal powder spray (we love Tinaderm for that) each time after use.
If you put in the hard work, you will see results. But, if you don’t, we would know – even if you say you do. It’s like when we go to the dentist and get asked whether we floss daily, and we say yes, when we actually mean yes for the last few days before the appointment. Ultimately, how consistent you are with the fungal nail treatment at home will determine how soon you will see results.
Final Thoughts
Fungal toenail infection is a very common dermatological condition we see as podiatrists. More often than not, we see co-occurrence of tinea pedis in individuals with fungal toenail infection. Therefore, when it comes to fungal nail treatment, it is always important to treat the nails, skin, as well as, the environment (shoes, socks, partner).
During the course of fungal nail treatment, our role as podiatrist is more like a facilitator – you do the home treatment at home daily, we see you every 4 weeks to give your toenails a good clean, monitor your progress and cheer you on.
Your fungal nail treatment outcome is as much your podiatrist’s input as yours. When your toenails are healthy and beautiful again, the credit belongs to yourself much more than us. And, we can’t wait to celebrate with you!
So, here are the three things we think you should know about fungal toenail infection. Other than fungal toenails, warts are another common dermatological condition we see at the clinic. And, of course, heel pain is also under our department.
We hope you have enjoyed reading this blogpost and learned a few things. If you need help with your feet, or know someone who does, why not get in touch with us today?
It’s lovely having you around. Till next time!




